
Male mice were infected with Zika virus and then mated with female mice. Efficient sexual transmission of the virus from males to females was observed. This observation in itself is very interesting but is not the focus of my comments.
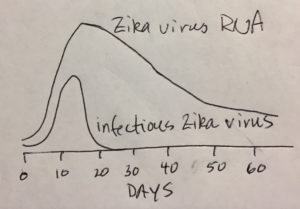
To understand the dynamics of sexual transmission, the authors measured Zika virus shedding in seminal fluid – by both PCR, to detect viral RNA, and by plaque assay, to detect infectious virus. The results are surprising (see figure – drawn in my hotel room).
Zika virus RNA persisted in semen for up to 60 days – far longer than did infectious virus, which could not be detected after about three weeks.
Many laboratories choose to assay the presence of viral genomes by PCR. This is an acceptable technique as long as the limitations are understood – it detects nucleic acids, not infectious virus.
Despite the presence of Zika virus RNA in seminal fluid for at least 60 days after infection, these mice are not likely to transmit virus after a few weeks. There is a lower limit of detection of the plaque assay – approximately 10 plaque forming units/ml – whether that would be sufficient to transmit infection is a good question.
Why Zika viral RNA and not infectious virus would persist for so long is an important and unanswered question that should definitely be studied.
Recently many papers have been published which demonstrate that Zika virus and Ebolavirus can persist in a variety of human fluids for extended periods of time. These results have been interpreted with alarm, both by scientists and by science writers. However, in most cases the assays were done by PCR, not by plaque assay, and therefore we do not know if infectious virus is present. Viral RNA would not constitute a threat to transmission, while infectious virus would.
The lesson from this study is very clear – in novel experimental or epidemiological studies it is important to prove that any viral nucleic acid detected by PCR is actually infectious virus. Failing to do so clouds the conclusions of the study.
There are few excuses for failing to measure viral infectivity by plaque assays. Please don’t tell me it’s too much work – that’s a poor excuse on which to base selection of an assay. Even if your virus doesn’t form plaques there are alternatives for measuring infectious virus.
If you are wondering how a plaque assay is done, check out my short video below.

Vincent, I was told awhile back that + strand RNA virus genetic material could be infectious on its own as it is effectively mRNA, so that were it to get into a host cell it could still be used on its own to make infectious virus. Is this actually the case, it could but would be rare? What you are saying here makes logical sense to me regardless of the answer to this, presence of RNA alone wouldn’t be proof it is actively doing anything infectious. But I want to make sure I don’t explain +strand RNA viruses inaccurately!
I’m not sure how you can get mRNA (viral or otherwise) to ribosomes inside a cell without using endosomal/fusion pathway. I don’t know very much, but I believe this requires quite complex mechanisms involving specific cell receptors and can’t be done by nucleic acids alone. But maybe I’m mistaken.
Using cellular vesicles perhaps? http://jvi.asm.org/content/89/24/12242.full
(+) strand RNA is indeed infectious, but only when introduced into cells under certain conditions. Such RNA is not infectious under the conditions of a plaque assay, nor is it likely to initiate infection in another person by transmission. The non-infectious RNA detected by plaque assay is likely fragments of RNA, not the entire genome – PCR only assays for short stretches of RNA.
Dear Proff.
I want to know if anything of this can relate with HIV, because PCR is not used to diagnosis, I’m not sure why but it has anything to do with this???
Vesicles acting like some sort of pseudovirions… That’s interesting. Thanks for the link!
Pingback: Viral RNA is not infectious virus! | virology |...
Pingback: parasitology | [Veterinary and Medical Sciences
Pingback: Viral RNA is not infectious virus! – Virology